When detected early, risks from serious eye diseases with significant personal, economic, and workplace costs are manageable
Twentieth Century philosopher John Dewey wrote, “A problem well put is half solved.” Group benefit stakeholders recognize the need for modernization of vision care and have asked the Canadian Association of Optometrists (CAO) for more details on where the gaps in vision care exist to develop effective solutions. The CAO’s blogs and webinars are addressing this knowledge gap and the CAO is developing additional resources that stakeholders can use to educate internal and external partners as they move forward.
“Almost everyone will experience impaired vision or an eye condition during their lifetime and require eye care services”
– The Lancet Global Health Commission on Global Eye Health
“People who need eye care must be able to receive high-quality interventions without suffering financial hardship”
– Dr. Tedros Adhanom Ghebreyesus, director-general, World Health Organization
Modern diagnostic tools provide valuable resources to optometrists during comprehensive and recall examinations in detecting patients’ risk and diagnosing serious eye diseases like macular degeneration, diabetic retinopathy, ocular surface disease, and glaucoma. They are also important for tracking and management of ocular manifestations of systemic diseases like diabetes and high hypertension. Plan members rely on group vision care benefits for coverage of diagnostics and examinations. Most public provincial and territorial health plans do not reimburse expenses for comprehensive examinations or diagnostics for working age residents and there are gaps in coverage for ongoing monitoring and disease management after a diagnosis.
Most current vision care plans fall short of providing adequate coverage to plan members in ways that may be surprising:
- The customary allowance for comprehensive examinations may be sufficient, but there is often no additional allowance for administration of necessary further diagnostics.
- There is generally no allowance for recall examinations for monitoring those at risk of serious eye disease.
Plan sponsors who move group vision care coverage from their insured health benefits plan to a qualifying healthcare spending account (HCSA) have an even larger gap. Vision care starts to compete against other eligible expenses within a finite benefit dollar amount.
However, gaps in vision care benefits do impact plan members.
During a CAO webinar, Dr. Andre Stanberry, clinic director and associate clinical professor of optometry at the University of Waterloo, identified three serious eye diseases that are common among those under age 60 and, therefore, have significant personal, economic, and workplace costs. When diagnosed early, these diseases are manageable and treatments to slow the progression of vision loss are usually very effective. They are:
•Glaucoma ‒ Approximately 76,000 Canadians under 60 have vision loss due to glaucoma and only half of people with glaucoma are diagnosed. The most common form of glaucoma results from the buildup of pressure from excess fluid within the eye. This leads to progressive damage of the optic nerve and reduced peripheral vision. At an early stage, treatment with medicated eye drops and/or laser surgery are used to control or prevent further vision loss. If left untreated, permanent and progressive vision loss will be likely to occur.
•Age-related Macular Degeneration (AMD) ‒ Approximately 25,000 Canadians under 60 have vision loss due to AMD.3 AMD results from damage to the macula, blurring central vision and causing it to deteriorate over time. Early detection and management can significantly slow its progression and prevent vision loss.
•Diabetic Retinopathy (DR) ‒ Approximately 71,000 Canadians under 60 have vision loss due to DR and rates of diabetes are climbing. Studies have shown that nearly everyone with type I diabetes develops DR within approximately 20 to 25 years. Today one in three Canadians have diabetes or pre-diabetes and the numbers are forecast to increase. An estimated 50 per cent of non-First Nations Canadians of young age and an estimated 80 per cent of First Nations people of young age will develop diabetes in their lifetime. Diabetic Retinopathy is a microvascular disease caused by high blood sugar, which results in the weakening or swelling of the tiny blood vessels that nourish the retina. This leads to blood leakage, the growth of new blood vessels, blood vessels that become blocked, and death to parts of the retina. If diabetic retinopathy is left untreated, it will lead to blindness. Treatment is much more effective if DR is detected at an early stage.
Modern Diagnostic Tools
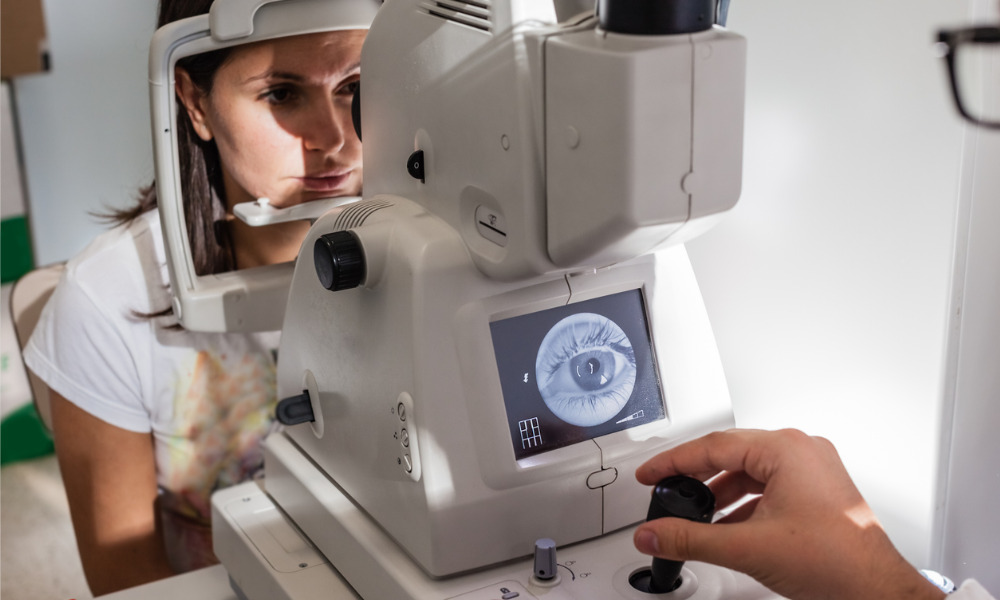
The purpose of several diagnostic tools used by optometrists is to identify structural and functional changes in the eye. Using these tools can identify risk factors and diagnose eye diseases that, if left undetected, will result in vision loss. Used during comprehensive and recall examinations, these tools play a key role in identifying and monitoring those with risk factors and in diagnosing, monitoring, and managing eye disease. Two important diagnostics ‒ the optical coherence tomography (OCT) scan and the visual field test ‒ work together for diagnosing and managing serious eye diseases.
OCT detects structural changes in the eye well before symptoms or functional deficiency start to happen. The OCT allows the optometrist to look directly into the layers at the back of the eye (retina) with high resolution. When there are signs of disease, the structural integrity of these layers will change. This is picked up from the OCT scan.
Optometrists use OCT scans during comprehensive and recall examinations. A baseline scan is recommended for all patients during an initial comprehensive examination and at every comprehensive examination when an optometrist determines there is reason to screen for diseases such as glaucoma, AMD, and DR. An OCT is also used during recall examinations when an initial scan indicates that frequent monitoring for changes is required, usually every three to six months between com- prehensive examinations. After a disease is diagnosed, an OCT scan may be part of the ongoing disease monitoring and management process.
Visual field tests can detect functional changes before an individual notices any changes to their field of vision. The visual field test compares results to established standards of what is considered ‘normal.’ Results of visual field testing can also deter- mine if someone meets the legal driving standards as well as identify certain neurological conditions and determine visual function after a stroke or trauma from, for example, a car accident or sports injury.
Optometrists use visual field tests during comprehensive examinations and during recall examinations when there is reason to monitor for signs of glaucoma, usually every three to six months between comprehensive examinations. If glaucoma is diagnosed, a visual field test may be part of the ongoing monitoring and management process.
While there have been significant developments in vision diagnostics, group vision care coverage has remained relatively unchanged. Modern optometry tools, when they are eligible for reimbursement, are often included within the standard comprehensive examination benefit maximum. This can mean reimbursement for diagnostic tools is limited, if it exists at all. Recall examinations are not typically considered eligible expenses.
Across Canada there is no provincial or territorial coverage for comprehensive eye examinations for people 20 to 64 years of age unless they have a diagnosis of a serious eye condition or are on social assistance. Public funding for advanced vision care intervention with a diagnosis of a serious eye condition varies across provinces and territories, not only in the types of care, patients, or conditions funded, but also in the amount or level of coverage they provide. For example, some provinces may cover the entire cost of a service, while others may reimburse a percentage of the cost or a percentage of the cost up to a maximum dollar amount. Therefore, the existence of public funding in a province does not eliminate access barriers for these vision care services. There are clear gaps in medically necessary vision care services for working Canadians. Insurers and plan sponsors should make filling the gaps in vision care a priority to:
- Improve employee satisfaction ‒ two-thirds of Canadians say that they are concerned about their eye health.
- Reduce presenteeism and disability ‒ a plan member who can’t see properly will not be as productive. If disease is diagnosed only after the plan member notices changes in their vision, the opportunity to avoid significant vision loss and future disability may have been lost.
The CAO is encouraging the benefits community to adopt a more progressive approach to vision care and close the coverage gaps for plan members. In doing so, plan members will have improved access to necessary diagnostic tools and examinations that will lead to earlier diagnosis and help preserve their sight.
Denise Balch is Principal Consultant at Connex. Ibrahim Daibes is Director of Policy and Research at the Canadian Association of Optometrists.



